Case History
Case number: 00003
A middle-aged tourist who arrived here after a six-hour flight is referred to the Emergency Department for left lower limb swelling. En route to the hospital, she had a witnessed, generalised tonic-clonic seizure. She is a heavy smoker; past medical history is otherwise unremarkable. She has no history of thrombosis or bleeding; previous pregnancies were uncomplicated and there were no miscarriages. On arrival in the ED, she started complaining of bilateral flank pain. She was hypotensive and required fluid resuscitation
Prior to admission, she had been well, with no inter-current illnesses. On review in the ED, she denies breathlessness or chest pain, be did have significant back pain. She was hypotensive, with a swollen left calf.
Investigations
Hb 15.4 TW 13.2 Plt 207
Cr 105
PT 13.4 (normal) APTT 23.8 (shorter than normal)
LFT normal
Anti-thrombin III 121%
Protein C 106%
Protein S 10%
Lupus anticoagulant, anti-B2 glycoprotein, anti-cardiolipin antibodies absent
Factor V Leiden homozygous normal
Jak2 V617F not detected
PNH screen negative
Homocysteine normal
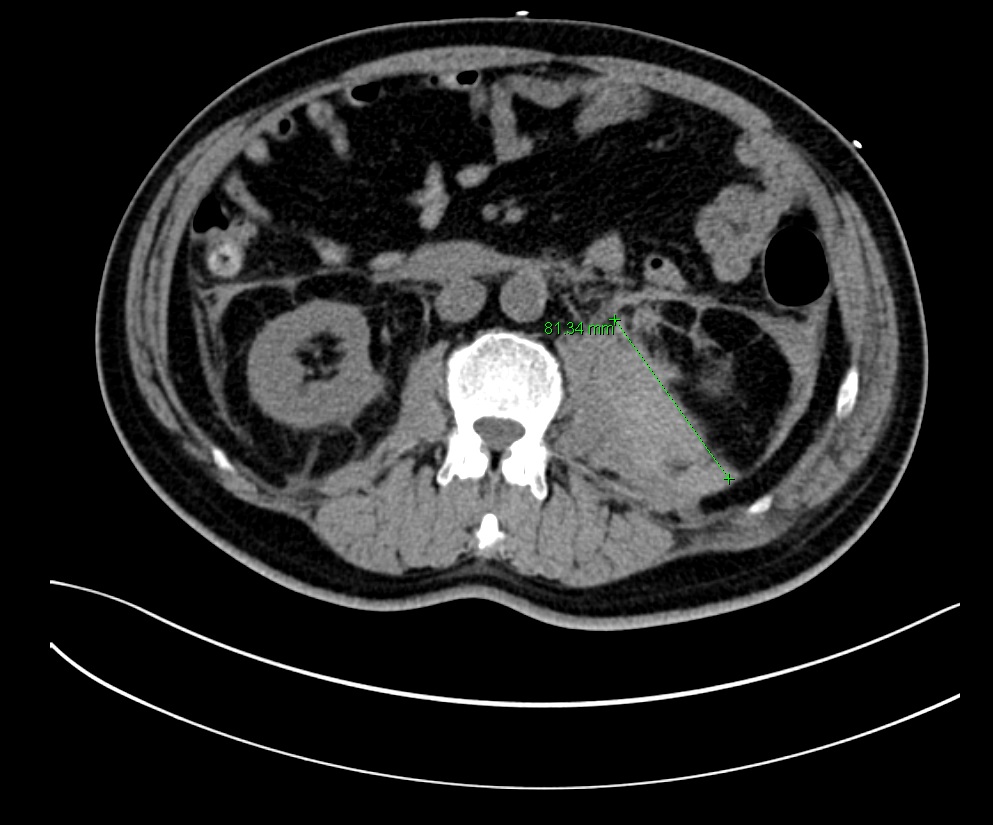
CT Aortogram showed no evidence of aortic dissection, but incidentally showed multiple pulmonary emboli and a large haematoma along the left psoas muscle, extending into the pelvis (7.5 x 8.0 x 16.1 cm). There were also filling defect noted in the inferior vena cava, left external iliac/femoral vein, suspicious of thrombosis.
MRI brain: filling defects and reduced flow in the right transverse, sigmoid sinuses and IJV are in keeping with partial thrombosis and partial occlusion. No venous oedema, venous infarct or mass effect is noted.
US Doppler: thrombosis in the left popliteal vein, superficial femoral vein, common femoral vein and left external iliac vein.
Questions:
- Why is the APTT shortened?
- What is the role of thrombophilia testing in someone presenting with an unprovoked thrombosis?
- What is the role of IVC filter insertion in patients who cannot be anticoagulated?
- What conditions should be considered in unusual venous thrombosis (e.g. multiple or rare sites)?

Leave A Comment